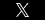Risk factors for Necrotizing fasciitis:
Clinical features:
There are local and systemic signs and symptoms of Necrotizing fasciitis:
Local signs and symptoms may include:
- Skin erythema.
- Skin edema (swelling).
- Skin ulceration with gangrenous edges.
- Skin necrosis.
- Skin numbness.
- Pain which is out of proportion to the degree of inflammation.
- Grayish-brown discharge.
- Vesicles, bullae.
- Crepitus (crackling or grating feeling or sound under the skin).
Systemic signs and symptoms may include:
- Fever.
- Chills.
- Hypotension (decrease blood pressure).
- Tachycardia (increased heart rate).
- Diaphoresis (excessive sweating).
- Hemodynamic instability.
- Altered mental status.
- Organ failure.
Diagnosis:
Necrotizing fasciitis is a life threatening rapidly expanding infection that can lead to systemic toxicity and death therefore early diagnosis and treatment is critical to reduce the risk of complications and death. Diagnosis include:
- Full history and physical examination including all parts of the body to search for skin inflammation.
- Lab work .
- Tissue biopsy which can reveal necrosis of deep tissues.
- Plain x-ray which can demonstrate subcutaneous gas.
- CT scan and MRI.
- Surgical exploration.
Differential Diagnosis:Diseases that may have similar features of necrotizing fasciitis include:
- Cellulitis.
- Erysipelas: an infection of the superficial dermis with well defined borders.
- Gas gangrene.
- Lymphangitis.
Treatment:
- Treatment of necrotizing fasciitis is composed of patient stabilization, surgical debridement and rapid administration of broad spectrum antibiotics. Some patient may need to be admitted to the intensive care unit for monitoring and treatment may involve an interdisciplinary care team. Patients are typically taken to surgery based on a high index of suspicion determined by the patient’s clinical features. During surgical debridement collection of tissue cultures and tissue samples are done for microscopic evaluation, excision of all nonviable tissue, and delineation of the extent of the disease. Multiple surgical debridement may be needed leaving a large opened wound which may reuire skin grafting.
- Intravenous antibiotics should be started as soon as necrotizing fasciitis is suspected. Wide spectrum antibiotics are usually used.
- Amputation of the affected organ or organs may be needed.
- Hyperbaric oxygen may be used as an adjunct to surgery and antibiotics.
This information is not intended nor implied to be a substitute for professional medical advice; it should not be used during any medical emergency or for the diagnosis or treatment of any medical condition. Call 911 for all medical emergencies.
 Burn Injury Resource Center
Burn Injury Resource Center