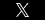Skin flap is a surgical procedure in which a healthy skin and its underlying subcutaneous tissue is taken from an area very close to the wound to be covered, the flap remains partly connected to its original site via its blood supply.
Skin graft is the surgical procedure in which a non healing wound or a burn wound is covered by a piece of healthy skin taken either from the patient or from a cadaver or an animal; the graft taken does not have its own blood supply and is completely separated from its original site . Skin graft is either used a temporary wound cover or a permanent one. Some wounds such as third degree burns if left to heal on their own can lead to scarring and contractions.
As the skin is the largest organ in the body and among its functions is playing a major role in protecting the body from fluid loss and help in preventing harmful micro organisims such as bacteria and viruses from entering the body and causing infections therefore its important to cover third degree burns with skin graft as soon as possible as uncovered third degree burns are more liable for wound infections and fluid loss from the burn area .